By Dr. Aswin Babu
Edited by Dr. Ahmed El-Medany
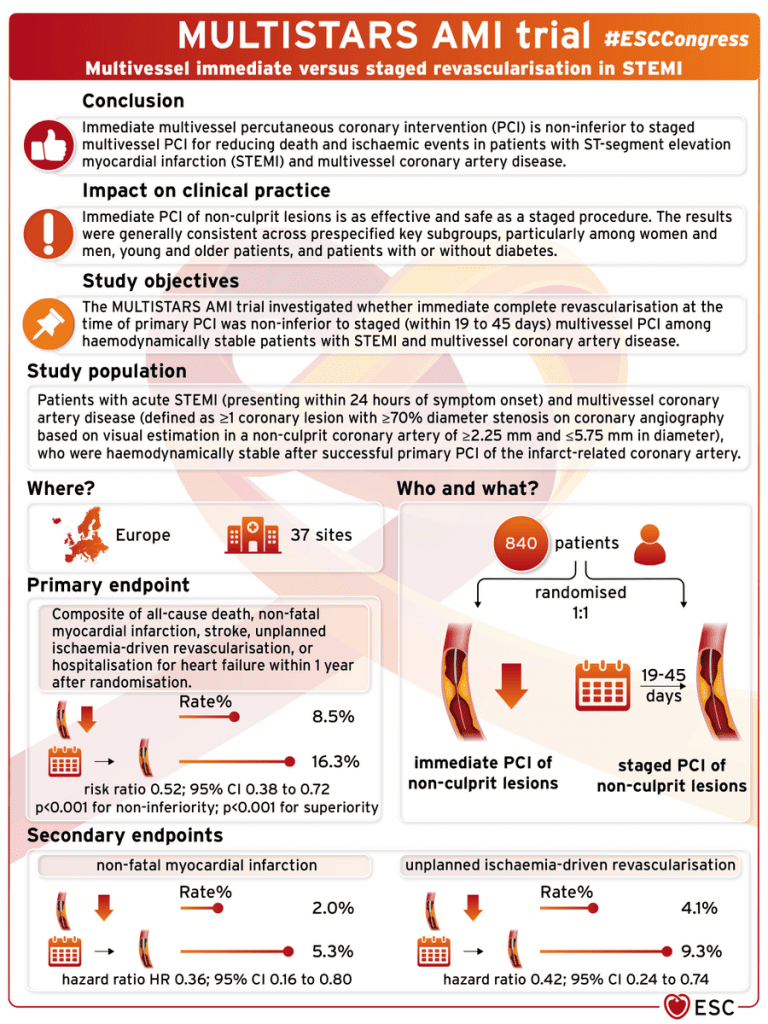
The MULTISTARS AMI trial (Figure 1) has set a new course in the landscape of cardiac care, unveiling the superiority of immediate percutaneous coronary intervention (PCI) over staged PCI in the treatment of ST-segment elevation myocardial infarction (STEMI) with multivessel coronary artery disease (CAD) in haemodynamically stable patients.
The primary objective of the trial was to assess the comparative safety and efficacy of immediate and staged PCI for non-culprit lesions in hemodynamically stable patients presenting with STEMI and multivessel CAD. In the immediate group, PCI to non-culprit lesions was performed during the index procedure. In the staged group, the intervention was deferred to a median of 37 days following the index PCI, within a window of 19-45 days. The use of fractional flow reserve (FFR) and intravascular ultrasound (IVUS) was left to the discretion of individual operators.
This was a randomised, open-label, multi-centre trial encompassing a total of 840 patients from 2,907 patients that were screened. 37 centres from Europe participated in this effort. Inclusion criteria included acute STEMI within 24 hours of symptom onset, multivessel CAD defined by angiographically relevant lesions (>70% stenosis in a vessel ≥2.25mm) and successful PCI of the culprit artery.
Patients were followed up for 30 months. The mean age was 65 years with 22% being female. The majority of patients were of white race (98%), and the location of myocardial infarction varied, with anterior (40%) and lateral (52%) regions accounting for a substantial proportion. The location of the non-culprit PCI was more pronounced in the left coronary system (left anterior descending 50%, left circumflex 46%).
The primary composite endpoint, incorporating all-cause mortality, nonfatal MI, stroke, unplanned ischemia-driven target lesion revascularisation (ID-TLR), and hospitalisation for heart failure at one year, demonstrated a compelling distinction between immediate and staged PCI. Immediate PCI boasted a significant 48% reduction in the primary endpoint when compared to staged PCI (8.5% vs 16.3%, RR 0.52, 95% CI 0.38-0.72; p for noninferiority < 0.001; p for superiority < 0.001).
In terms of secondary outcomes, there was no difference in the rates of all-cause mortality, stroke, or hospitalisation of heart failure between both cohorts. However, both non-fatal MI and ID-TLR were significantly more reduced in the immediate PCI arm (p < 0.05).
The results of the MULTISTARS AMI trial reveal the advantages of immediate PCI over staged PCI, with benefits predominantly driven by a reduction in nonfatal MI and ID-TLR. This phenomenon likely reflects the unstable environment generated throughout the coronary tree, stemming from inflammation in the culprit vessel. These findings resonate with the insights gleaned from the COMPLETE trial, emphasising the superiority of complete revascularisation over culprit-only revascularisation in haemodynamically stable STEMI patients with multivessel disease. Whilst the COMPLETE trial endorsed complete revascularisation during or after the index hospitalisation, the MULTISTARS AMI trial accentuates the advantage of immediate complete revascularisation during the index procedure. However, given the lack of mortality benefit, there needs to be further longitudinal studies assessing the timing of complete revascularisation during the index hospitalisation before a shift in guidelines and practice can be fully and confidently implemented.
Link to Article – https://www.nejm.org/doi/full/10.1056/NEJMoa2307823

