By Dr Jonathan Shurlock
Edited by Dr Ahmed El-Medany
Up to a third of patients undergoing transcatheter aortic valve implantation (TAVI) have concurrent moderate/severe mitral regurgitation (MR), contributing to a worse prognosis.
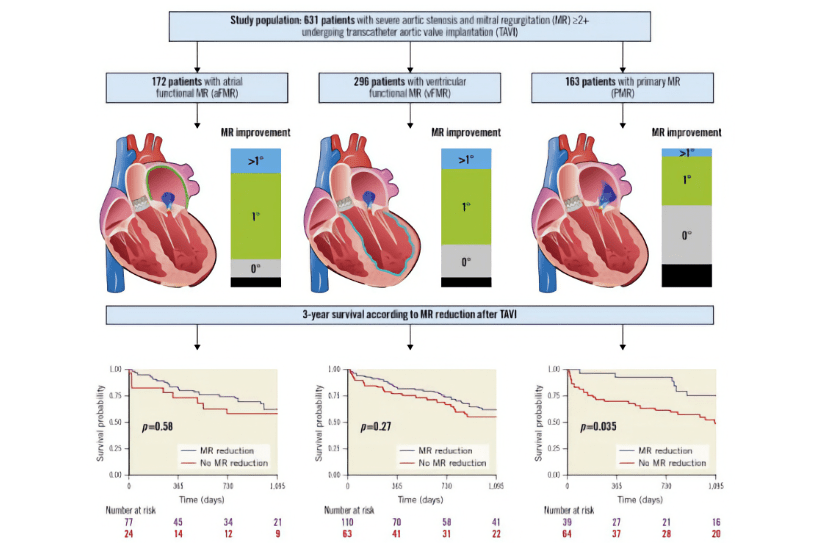
An interesting observational study in EuroIntervention has explored the impact of different MR aetiologies on individuals undergoing TAVI. Doldi et al. specifically focus on atrial functional MR (aFMR), ventricular functional MR (vFMR), and primary MR (PMR) and look at any changes seen post-TAVI.
The study draws from a patient database held at Munich University Hospital and included any patients undergoing TAVI, with at least moderate MR, between January 2013 and December 2020. MR aetiology was determined via echocardiographic assessment. Key outcome measures included 3-year mortality, change in MR severity, and NYHA score at follow up.
From a total of 3,474 individuals undergoing TAVI in the defined period, 631 had MR of at least moderate severity. These were subdivided into MR aetiology: 296 vFMR, 172 aFMR, 163 PMR. There was no difference in 3-year mortality post-TAVI between the 3 groups (p=0.57). The aFMR group had the greatest improvement in MR post-TAVI (80.2% versus vFMR: 69.4%, p=0.03, and PMR: 40.8%, p<0.001). Interestingly, despite no difference in 3-year mortality the authors did find an association between persistence of MR at follow up and increased mortaility (hazard ratio 1.49, 95% CI 1.04-2.11; p=0.027). NYHA score improved significantly in all groups. In summary of the 3 groups, PMR was associated with the least improvement in MR, least symptomatic improvement, and most importantly lowest survival rates post-TAVI.
These findings demonstrate the complex relationship between aetiology of MR in the context of individuals undergoing TAVI, with clear implications for mortality and morbidity. Studies such as this, while small, add essential evidence to enable a more informed discussion with patients when discussing invasive interventions including TAVI.
Full study here: https://eurointervention.pcronline.com/article/impact-of-mitral-regurgitation-aetiology-on-the-outcomes-of-transcatheter-aortic-valve-implantation